Search
- Page Path
- HOME > Search
- Thyroid
Thyroid Cancer Screening - Cost-Utility Analysis of Early Detection with Ultrasonography of Differentiated Thyroid Cancer: A Retrospective Study on a Korean Population
- Han-Sang Baek, Jeonghoon Ha, Kwangsoon Kim, Ja Seong Bae, Jeong Soo Kim, Sungju Kim, Dong-Jun Lim, Chul-Min Kim
- Endocrinol Metab. 2024;39(2):310-323. Published online April 9, 2024
- DOI: https://doi.org/10.3803/EnM.2023.1870
- 401 View
- 11 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
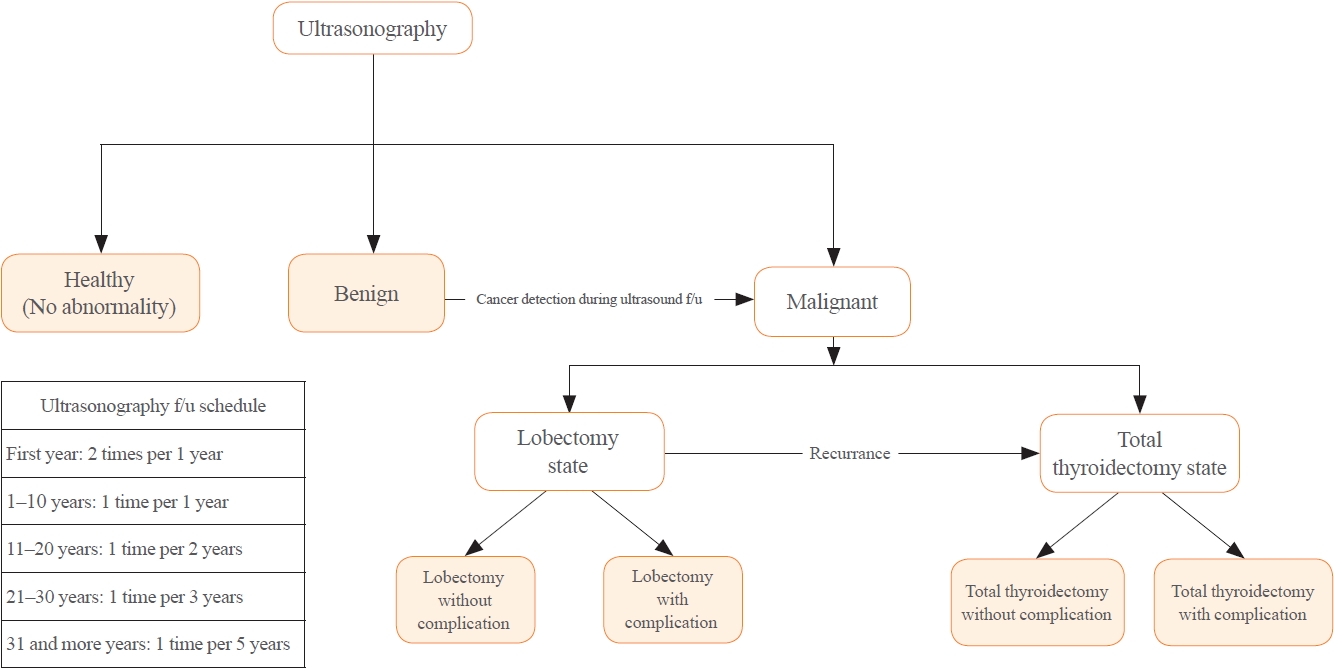
There is debate about ultrasonography screening for thyroid cancer and its cost-effectiveness. This study aimed to evaluate the cost-effectiveness of early screening (ES) versus symptomatic detection (SD) for differentiated thyroid cancer (DTC) in Korea.
Methods
A Markov decision analysis model was constructed to compare the cost-effectiveness of ES and SD. The model considered direct medical costs, health outcomes, and different diagnostic and treatment pathways. Input data were derived from literature and Korean population studies. Incremental cost-effectiveness ratio (ICER) was calculated. Willingness-to-pay (WTP) threshold was set at USD 100,000 or 20,000 per quality-adjusted life year (QALY) gained. Sensitivity analyses were conducted to address uncertainties of the model’s variables.
Results
In a base case scenario with 50 years of follow-up, ES was found to be cost-effective compared to SD, with an ICER of $2,852 per QALY. With WTP set at $100,000, in the case with follow-up less than 10 years, the SD was cost-effective. Sensitivity analysis showed that variables such as lobectomy probability, age, mortality, and utility scores significantly influenced the ICER. Despite variations in costs and other factors, all ICER values remained below the WTP threshold.
Conclusion
Findings of this study indicate that ES is a cost-effective strategy for DTC screening in the Korean medical system. Early detection and subsequent lobectomy contribute to the cost-effectiveness of ES, while SD at an advanced stage makes ES more cost-effective. Expected follow-up duration should be considered to determine an optimal strategy for DTC screening.

- Diabetes, obesity and metabolism
Big Data Articles (National Health Insurance Service Database) - Long-Term Cumulative Exposure to High γ-Glutamyl Transferase Levels and the Risk of Cardiovascular Disease: A Nationwide Population-Based Cohort Study
- Han-Sang Baek, Bongseong Kim, Seung-Hwan Lee, Dong-Jun Lim, Hyuk-Sang Kwon, Sang-Ah Chang, Kyungdo Han, Jae-Seung Yun
- Endocrinol Metab. 2023;38(6):770-781. Published online November 6, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1726
- 1,112 View
- 48 Download
- 1 Web of Science
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
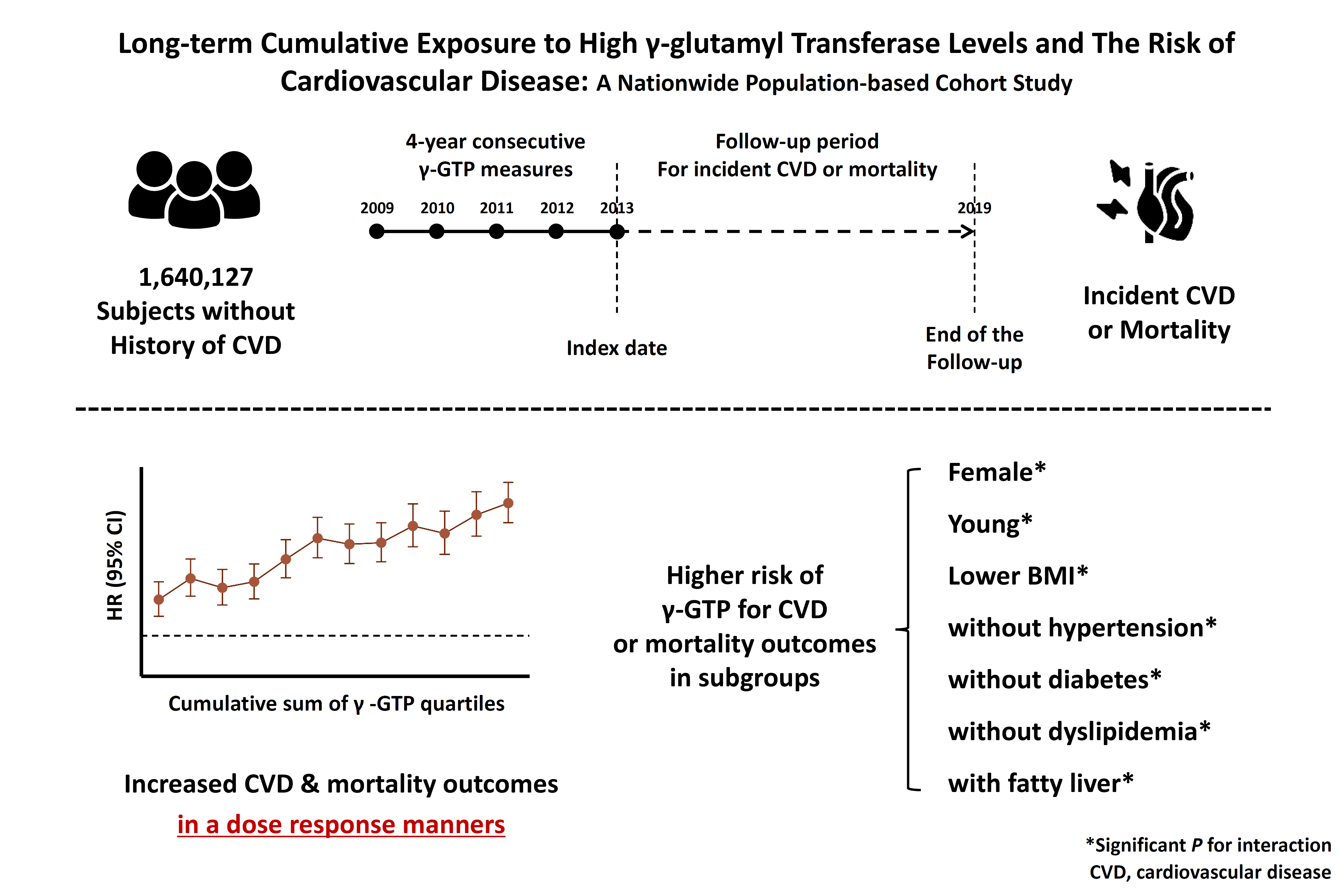
Elevated γ-glutamyl transferase (γ-GTP) levels are associated with metabolic syndrome. We investigated the association of cumulative exposure to high γ-GTP with the risk of cardiovascular disease (CVD) in a large-scale population.
Methods
Using nationally representative data from the Korean National Health Insurance system, 1,640,127 people with 4 years of consecutive γ-GTP measurements from 2009 to 2012 were included and followed up until the end of 2019. For each year of the study period, participants were grouped by the number of exposures to the highest γ-GTP quartile (0–4), and the sum of quartiles (0–12) was defined as cumulative γ-GTP exposure. The hazard ratio for CVD was evaluated using the Cox proportional hazards model.
Results
During the 6.4 years of follow-up, there were 15,980 cases (0.97%) of myocardial infarction (MI), 14,563 (0.89%) of stroke, 29,717 (1.81%) of CVD, and 25,916 (1.58%) of death. Persistent exposure to high γ-GTP levels was associated with higher risks of MI, stroke, CVD, and death than those without such exposure. The risks of MI, stroke, CVD, and mortality increased in a dose-dependent manner according to total cumulative γ-GTP (all P for trend <0.0001). Subjects younger than 65 years, with a body mass index <25 kg/m2, and without hypertension or fatty liver showed a stronger relationship between cumulative γ-GTP and the incidence of MI, CVD, and death.
Conclusion
Cumulative γ-GTP elevation is associated with CVD. γ-GTP could be more widely used as an early marker of CVD risk, especially in individuals without traditional CVD risk factors.

- Thyroid
- Exploring the Association between Thyroid Function and Frailty: Insights from Representative Korean Data
- Youn-Ju Lee, Min-Hee Kim, Dong-Jun Lim, Jung-Min Lee, Sang Ah Chang, Jeongmin Lee
- Endocrinol Metab. 2023;38(6):729-738. Published online November 2, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1769
- 1,100 View
- 73 Download
- 1 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
This study investigates the association between thyroid function and frailty in the old patients using representative data.
Methods
The study was conducted using data from the Korea National Health and Nutrition Examination Survey conducted from 2013 to 2015. The study population included 2,416 participants aged 50 years and older with available thyroid function test data. Frailty assessment was performed using the Fried frailty phenotype. The prevalence of frailty was analyzed across different thyroid diseases and thyroid function parameters.
Results
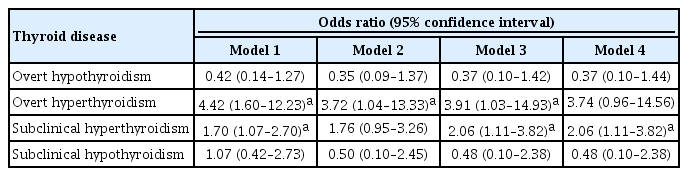
The significant association between thyroid dysfunction and frailty was observed in overt hyperthyroidism and subclinical hyperthyroidism. After adjusting for various factors, the association between thyroid dysfunction and frailty remained significant. On the other hand, overt hypothyroidism did not show a significant association with frailty in the adjusted analysis. For individuals with overt hyperthyroidism and subclinical hyperthyroidism, higher levels of free thyroxine (FT4) were significantly associated with an increased risk of frailty (aOR >999; 95% CI, >999 to 999). Among individuals with overt hypothyroidism, lower level of FT4 levels and high thyrotropin (TSH) levels showed a significant association with frailty risk (FT4: aOR, <0.01; TSH: aOR, 999). In participants with subclinical hypothyroidism, there were no significant associations between parameters for thyroid and frailty risk.
Conclusion
These findings suggest that thyroid dysfunction, particularly overt hyperthyroidism and subclinical hyperthyroidism, may be associated with an increased risk of frailty in the old patients. -
Citations
Citations to this article as recorded by- Associations of thyroid feedback quantile-based index with diabetes in euthyroid adults in the United States and China
Heng Wan, Genfeng Yu, Yajun He, Siyang Liu, Xingying Chen, Yuqi Jiang, Hualin Duan, Xu Lin, Lan Liu, Jie Shen
Annals of Medicine.2024;[Epub] CrossRef
- Associations of thyroid feedback quantile-based index with diabetes in euthyroid adults in the United States and China

- Thyroid
- The Early Changes in Thyroid-Stimulating Immunoglobulin Bioassay over Anti-Thyroid Drug Treatment Could Predict Prognosis of Graves’ Disease
- Jin Yu, Han-Sang Baek, Chaiho Jeong, Kwanhoon Jo, Jeongmin Lee, Jeonghoon Ha, Min Hee Kim, Jungmin Lee, Dong-Jun Lim
- Endocrinol Metab. 2023;38(3):338-346. Published online June 9, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1664
- 1,733 View
- 102 Download
- 1 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
To determine whether baseline thyroid-stimulating immunoglobulin (TSI) bioassay or its early response upon treatment with an anti-thyroid drug (ATD) can predict prognosis of Graves’ disease (GD) in real-world practice.
Methods
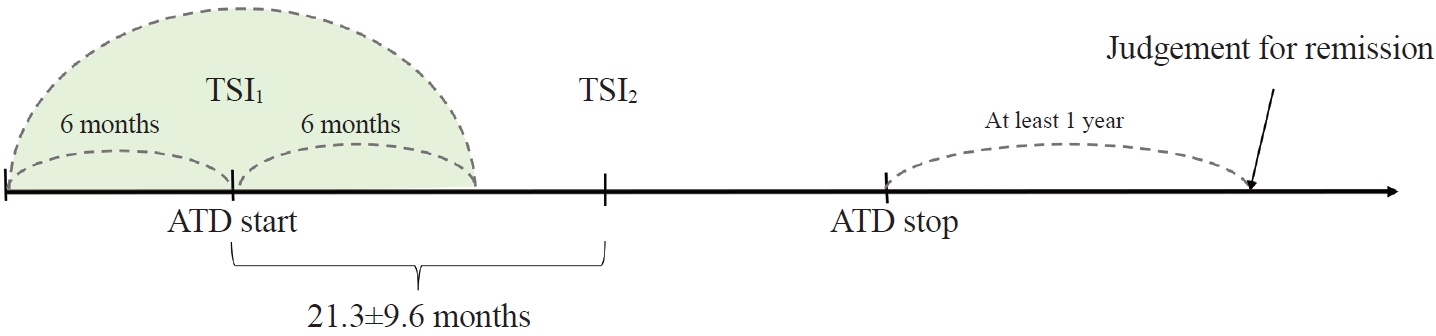
This retrospective study enrolled GD patients who had previous ATD treatment with TSI bioassay checked at baseline and at follow-up from April 2010 to November 2019 in one referral hospital. The study population were divided into two groups: patients who experienced relapse or continued ATD (relapse/persistence), and patients who experienced no relapse after ATD discontinuation (remission). The slope and area under the curve at 1st year (AUC1yr) of thyroid-stimulating hormone receptor antibodies including TSI bioassay and thyrotropin-binding inhibitory immunoglobulin (TBII) were calculated as differences between baseline and second values divided by time duration (year).
Results
Among enrolled 156 study subjects, 74 (47.4%) had relapse/persistence. Baseline TSI bioassay values did not show significant differences between the two groups. However, the relapse/persistence group showed less decremental TSI bioassay in response to ATD than the remission group (–84.7 [TSI slope, –198.2 to 8.2] vs. –120.1 [TSI slope, –204.4 to –45.9], P=0.026), whereas the TBII slope was not significantly different between the two groups. The relapse/persistence group showed higher AUC1yr of TSI bioassay and TBII in the 1st year during ATD treatment than the remission group (AUC1yr for TSI bioassay, P=0.0125; AUC1yr for TBII,P =0.001).
Conclusion
Early changes in TSI bioassay can better predict prognosis of GD than TBII. Measurement of TSI bioassay at beginning and follow-up could help predict GD prognosis. -
Citations
Citations to this article as recorded by- Enhanced predictive validity of integrative models for refractory hyperthyroidism considering baseline and early therapy characteristics: a prospective cohort study
Xinpan Wang, Tiantian Li, Yue Li, Qiuyi Wang, Yun Cai, Zhixiao Wang, Yun Shi, Tao Yang, Xuqin Zheng
Journal of Translational Medicine.2024;[Epub] CrossRef - Long-term effect of thyrotropin-binding inhibitor immunoglobulin on atrial fibrillation in euthyroid patients
Jung-Chi Hsu, Kang-Chih Fan, Ting-Chuan Wang, Shu-Lin Chuang, Ying-Ting Chao, Ting-Tse Lin, Kuan-Chih Huang, Lian-Yu Lin, Lung-Chun Lin
Endocrine Practice.2024;[Epub] CrossRef
- Enhanced predictive validity of integrative models for refractory hyperthyroidism considering baseline and early therapy characteristics: a prospective cohort study

- Diabetes, Obesity and Metabolism
- Characteristics of Glycemic Control and Long-Term Complications in Patients with Young-Onset Type 2 Diabetes (Endocrinol Metab 2022;37:641-51, Han-sang Baek et al.)
- Han-sang Baek, Ji-Yeon Park, Jin Yu, Joonyub Lee, Yeoree Yang, Jeonghoon Ha, Seung Hwan Lee, Jae Hyoung Cho, Dong-Jun Lim, Hun-Sung Kim
- Endocrinol Metab. 2022;37(6):945-946. Published online December 2, 2022
- DOI: https://doi.org/10.3803/EnM.2022.602
- [Original]
- 1,733 View
- 165 Download

- Diabetes, Obesity and Metabolism
- Characteristics of Glycemic Control and Long-Term Complications in Patients with Young-Onset Type 2 Diabetes
- Han-sang Baek, Ji-Yeon Park, Jin Yu, Joonyub Lee, Yeoree Yang, Jeonghoon Ha, Seung Hwan Lee, Jae Hyoung Cho, Dong-Jun Lim, Hun-Sung Kim
- Endocrinol Metab. 2022;37(4):641-651. Published online August 29, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1501
- 6,168 View
- 166 Download
- 10 Web of Science
- 8 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
The prevalence of young-onset diabetes (YOD) has been increasing worldwide. As the incidence of YOD increases, it is necessary to determine the characteristics of YOD and the factors that influence its development and associated complications.
Methods
In this retrospective study, we recruited patients who were diagnosed with type 2 diabetes mellitus between June 2001 and December 2021 at a tertiary hospital. The study population was categorized according to age: YOD (age <40 years), middle-age-onset diabetes (MOD, 40≤ age <65 years), and late-onset diabetes (LOD, age ≥65 years). We examined trends in glycemic control by analyzing fasting glucose levels during the first year in each age group. A Cox proportional-hazards model was used to determine the relative risk of developing complications according to glycemic control trends.
Results
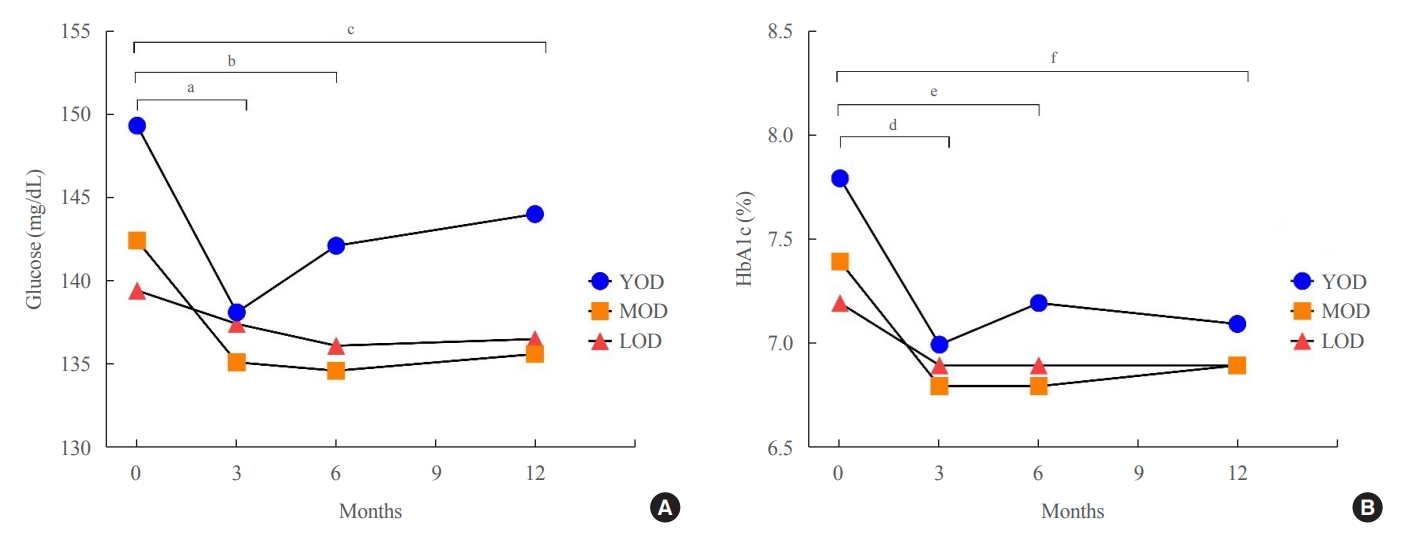
The fasting glucose level at the time of diagnosis was highest in the YOD group (YOD 149±65 mg/dL; MOD 143±54 mg/dL; and LOD 140±55 mg/dL; p=0.009). In the YOD group, glucose levels decreased at 3 months, but increased by 12 months. YOD patients and those with poor glycemic control in the first year were at a higher risk of developing complications, whereas the risk in patients with LOD was not statistically significant.
Conclusion
YOD patients had higher glucose levels at diagnosis, and their glycemic control was poorly maintained. As poor glycemic control can influence the development of complications, especially in young patients, intensive treatment is necessary for patients with YOD. -
Citations
Citations to this article as recorded by- Increased risk of incident mental disorders in adults with new-onset type 1 diabetes diagnosed after the age of 19: A nationwide cohort study
Seohyun Kim, Gyuri Kim, So Hyun Cho, Rosa Oh, Ji Yoon Kim, You-Bin Lee, Sang-Man Jin, Kyu Yeon Hur, Jae Hyeon Kim
Diabetes & Metabolism.2024; 50(1): 101505. CrossRef - Association between age at diagnosis of type 2 diabetes and cardiovascular morbidity and mortality risks: A nationwide population-based study
Da Hea Seo, Mina Kim, Young Ju Suh, Yongin Cho, Seong Hee Ahn, Seongbin Hong, So Hun Kim
Diabetes Research and Clinical Practice.2024; 208: 111098. CrossRef - Impact of diabetes distress on glycemic control and diabetic complications in type 2 diabetes mellitus
Hye-Sun Park, Yongin Cho, Da Hea Seo, Seong Hee Ahn, Seongbin Hong, Young Ju Suh, Suk Chon, Jeong-Taek Woo, Sei Hyun Baik, Kwan Woo Lee, So Hun Kim
Scientific Reports.2024;[Epub] CrossRef - Early onset type 2 diabetes mellitus: an update
Myrsini Strati, Melpomeni Moustaki, Theodora Psaltopoulou, Andromachi Vryonidou, Stavroula A. Paschou
Endocrine.2024;[Epub] CrossRef - Complications and Treatment of Early-Onset Type 2 Diabetes
Fahimeh Soheilipour, Naghmeh Abbasi Kasbi, Mahshid Imankhan, Delaram Eskandari
International Journal of Endocrinology and Metabolism.2023;[Epub] CrossRef - Characteristics of Glycemic Control and Long-Term Complications in Patients with Young-Onset Type 2 Diabetes (Endocrinol Metab 2022;37:641-51, Han-sang Baek et al.)
Han-sang Baek, Ji-Yeon Park, Jin Yu, Joonyub Lee, Yeoree Yang, Jeonghoon Ha, Seung Hwan Lee, Jae Hyoung Cho, Dong-Jun Lim, Hun-Sung Kim
Endocrinology and Metabolism.2022; 37(6): 945. CrossRef -
ISPAD
Clinical Practice Consensus Guidelines 2022: Management of the child, adolescent, and young adult with diabetes in limited resource settings
Anju Virmani, Stuart J. Brink, Angela Middlehurst, Fauzia Mohsin, Franco Giraudo, Archana Sarda, Sana Ajmal, Julia E. von Oettingen, Kuben Pillay, Supawadee Likitmaskul, Luis Eduardo Calliari, Maria E. Craig
Pediatric Diabetes.2022; 23(8): 1529. CrossRef - Characteristics of Glycemic Control and Long-Term Complications in Patients with Young-Onset Type 2 Diabetes (Endocrinol Metab 2022;37:641-51, Han-sang Baek et al.)
May Thu Hla Aye, Sajid Adhi Raja, Vui Heng Chong
Endocrinology and Metabolism.2022; 37(6): 943. CrossRef
- Increased risk of incident mental disorders in adults with new-onset type 1 diabetes diagnosed after the age of 19: A nationwide cohort study

- Thyroid
- Quality of Life of Survivors of Thyroid Cancer Is Not Inferior to That in Subjects without Cancer: Long-Term after Over 5 Years
- Jeongmin Lee, Youn-Ju Lee, Dong-Jun Lim, Jung-Min Lee, Sang-Ah Chang, Min-Hee Kim
- Endocrinol Metab. 2022;37(4):664-673. Published online August 29, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1499
- 3,163 View
- 183 Download
- 2 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Patients with thyroid cancer undergo less extensive surgery and additional therapies compared to those with other cancers. We aimed to compare the quality of life (QoL) between patients with thyroid cancer and healthy subjects using representative data from Korea. Differences in QoL of thyroid cancer survivors according to the duration after cancer diagnosis was also evaluated.
Methods
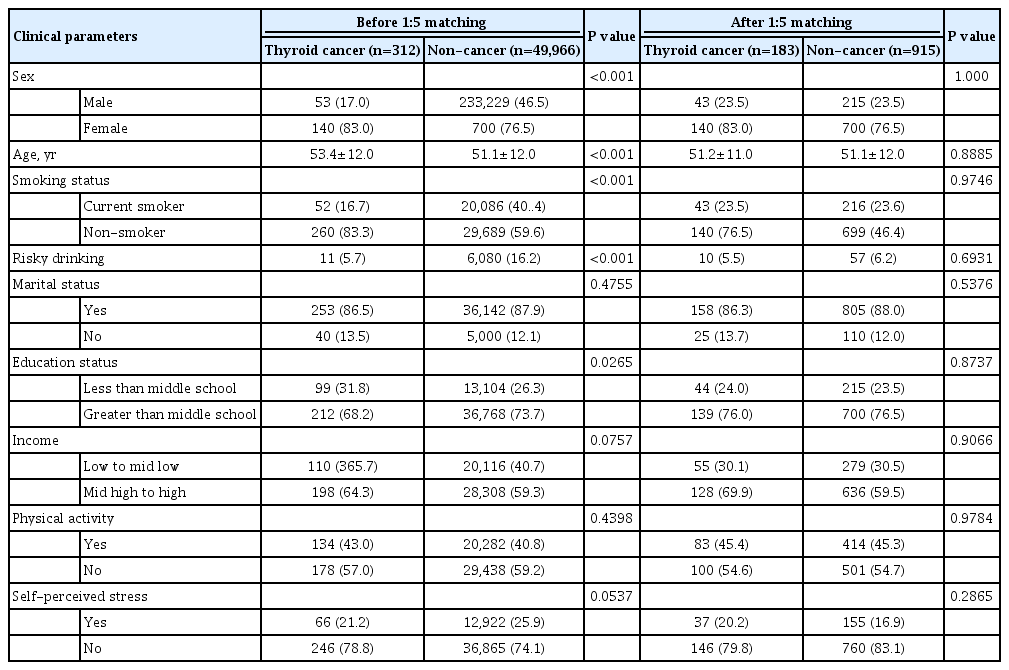
This population-based cohort study included 50,278 subjects who participated in the Korea National Health and Nutrition Examination Survey between 2007 and 2017. QoL was compared between patients with thyroid cancer and healthy subjects using self-reported data from the EuroQoL (EQ)-5 dimension (5D) and EQ-visual analog scale (VAS). Propensity score matching was used to match thyroid cancer survivors to healthy subjects (1:5 matching).
Results
Linear regression with univariate analysis showed that the presence of thyroid cancer was positively correlated with better EQ-5D index scores (β-coefficient=0.010, p=0.046). After adjusting for multiple covariables, statistical significance was maintained. EQ-VAS fails to demonstrate any significant correlation. Among the EQ-5D categories, patients with thyroid cancer showed better self-care than healthy subjects. Thyroid cancer duration did not correlate with the EQ-5D index score. In subgroup analyses, compared to patients with thyroid cancer duration of <5 years, no significant difference was observed in the correlation between the EQ-5D index score and survival duration in those with thyroid cancer duration of 5 to 9 years and ≥10 years.
Conclusion
Using a large-scale nationwide population-based database, our study demonstrated better QoL, especially in terms of self-care, among thyroid cancer survivors than among healthy subjects without cancer. -
Citations
Citations to this article as recorded by- Quality of Life Considerations in Patients Treated for Differentiated Thyroid Cancer
Jie Liu
Clinical Thyroidology.2023; 35(4): 160. CrossRef - The psychosocial impact of thyroid cancer
Parker Haymart, Nina Jackson Levin, Megan R. Haymart
Current Opinion in Endocrinology, Diabetes & Obesity.2023; 30(5): 252. CrossRef - Longitudinal Changes in Quality of Life Before and After Thyroidectomy in Patients With Differentiated Thyroid Cancer
Byung Hun Kim, Soo Rack Ryu, Jin Won Lee, Chang Myeon Song, Yong Bae Ji, Seok Hyun Cho, Seung Hwan Lee, Kyung Tae
The Journal of Clinical Endocrinology & Metabolism.2023;[Epub] CrossRef
- Quality of Life Considerations in Patients Treated for Differentiated Thyroid Cancer

- Thyroid
- Usefulness of Real-Time Quantitative Microvascular Ultrasonography for Differentiation of Graves’ Disease from Destructive Thyroiditis in Thyrotoxic Patients
- Han-Sang Baek, Ji-Yeon Park, Chai-Ho Jeong, Jeonghoon Ha, Moo Il Kang, Dong-Jun Lim
- Endocrinol Metab. 2022;37(2):323-332. Published online April 13, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1413
- 3,676 View
- 144 Download
- 4 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
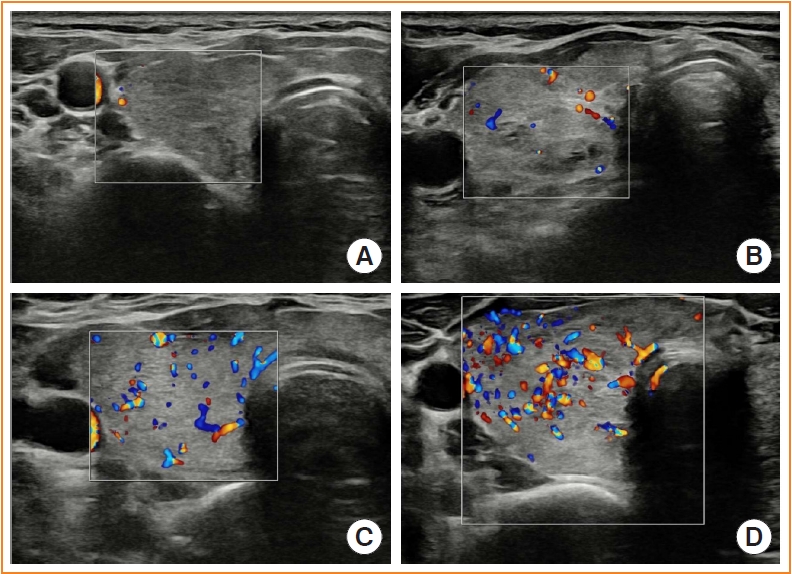
Microvascular ultrasonography (MVUS) is a third-generation Doppler technique that was developed to increase sensitivity compared to conventional Doppler. The purpose of this study was to compare MVUS with conventional color Doppler (CD) and power Doppler (PD) imaging to distinguish Graves’ disease (GD) from destructive thyroiditis (DT).
Methods
This prospective study included 101 subjects (46 GDs, 47 DTs, and eight normal controls) from October 2020 to November 2021. All ultrasonography examinations were performed using microvascular flow technology (MV-Flow). The CD, PD, and MVUS images were semi-quantitatively graded according to blood flow patterns. On the MVUS images, vascularity indices (VIs), which were the ratio (%) of color pixels in the total grayscale pixels in a defined region of interest, were obtained automatically. Receiver operating characteristic curve analysis was performed to verify the diagnostic performance of MVUS. The interclass correlation coefficient and Cohen’s kappa analysis were used to analyze the reliability of MVUS (ClinicalTrials.gov:NCT04879173).
Results
The area under the curve (AUC) for CD, PD, MVUS, and MVUS-VI was 0.822, 0.844, 0.808, and 0.852 respectively. The optimal cutoff value of the MVUS-VI was 24.95% for distinguishing GD and DT with 87% sensitivity and 80.9% specificity. We found a significant positive correlation of MVUS-VI with thyrotropin receptor antibody (r=0.554) and with thyroid stimulating immunoglobulin bioassay (r=0.841). MVUS showed high intra- and inter-observer reliability from various statistical method.
Conclusion
In a real time and quantitative manner, MVUS-VI could be helpful to differentiate GD from thyroiditis in thyrotoxic patients, with less inter-observer variability. -
Citations
Citations to this article as recorded by- Association of autoimmune thyroid disease with type 1 diabetes mellitus and its ultrasonic diagnosis and management
Jin Wang, Ke Wan, Xin Chang, Rui-Feng Mao
World Journal of Diabetes.2024; 15(3): 348. CrossRef - The Early Changes in Thyroid-Stimulating Immunoglobulin Bioassay over Anti-Thyroid Drug Treatment Could Predict Prognosis of Graves’ Disease
Jin Yu, Han-Sang Baek, Chaiho Jeong, Kwanhoon Jo, Jeongmin Lee, Jeonghoon Ha, Min Hee Kim, Jungmin Lee, Dong-Jun Lim
Endocrinology and Metabolism.2023; 38(3): 338. CrossRef - Duplex Hemodynamic Parameters of Both Superior and Inferior Thyroid Arteries in Evaluation of Thyroid Hyperfunction Disorders
Maha Assem Hussein, Alaa Abdel Hamid, Rasha M Abdel Samie, Elshaymaa Hussein, Shereen Sadik Elsawy
International Journal of General Medicine.2022; Volume 15: 7131. CrossRef - Case 5: A 41-Year-Old Woman With Palpitation
Jiwon Yang, Kabsoo Shin, Jeongmin Lee, Jeonghoon Ha, Dong-Jun Lim, Han-Sang Baek
Journal of Korean Medical Science.2022;[Epub] CrossRef - Microvascular assessment of fascio-cutaneous flaps by ultrasound: A large animal study
Guillaume Goudot, Yanis Berkane, Eloi de Clermont-Tonnerre, Claire Guinier, Irina Filz von Reiterdank, Antonia van Kampen, Korkut Uygun, Curtis L. Cetrulo, Basak E. Uygun, Anahita Dua, Alexandre G. Lellouch
Frontiers in Physiology.2022;[Epub] CrossRef
- Association of autoimmune thyroid disease with type 1 diabetes mellitus and its ultrasonic diagnosis and management

- Thyroid
- Lobeglitazone, A Peroxisome Proliferator-Activated Receptor-Gamma Agonist, Inhibits Papillary Thyroid Cancer Cell Migration and Invasion by Suppressing p38 MAPK Signaling Pathway
- Jun-Qing Jin, Jeong-Sun Han, Jeonghoon Ha, Han-Sang Baek, Dong-Jun Lim
- Endocrinol Metab. 2021;36(5):1095-1110. Published online October 14, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1155
- 4,743 View
- 159 Download
- 9 Web of Science
- 8 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
Peroxisome proliferator-activated receptor-gamma (PPAR-γ) ligands have been widely shown to correlate with epithelial-mesenchymal transition (EMT) and cancer progression. Lobeglitazone (LGZ) is a novel ligand of PPAR-γ; and its role in EMT and metastasis in papillary thyroid carcinoma (PTC) is poorly understood. We aimed to investigate the role of LGZ in metastatic behavior of PTC cells.
Methods
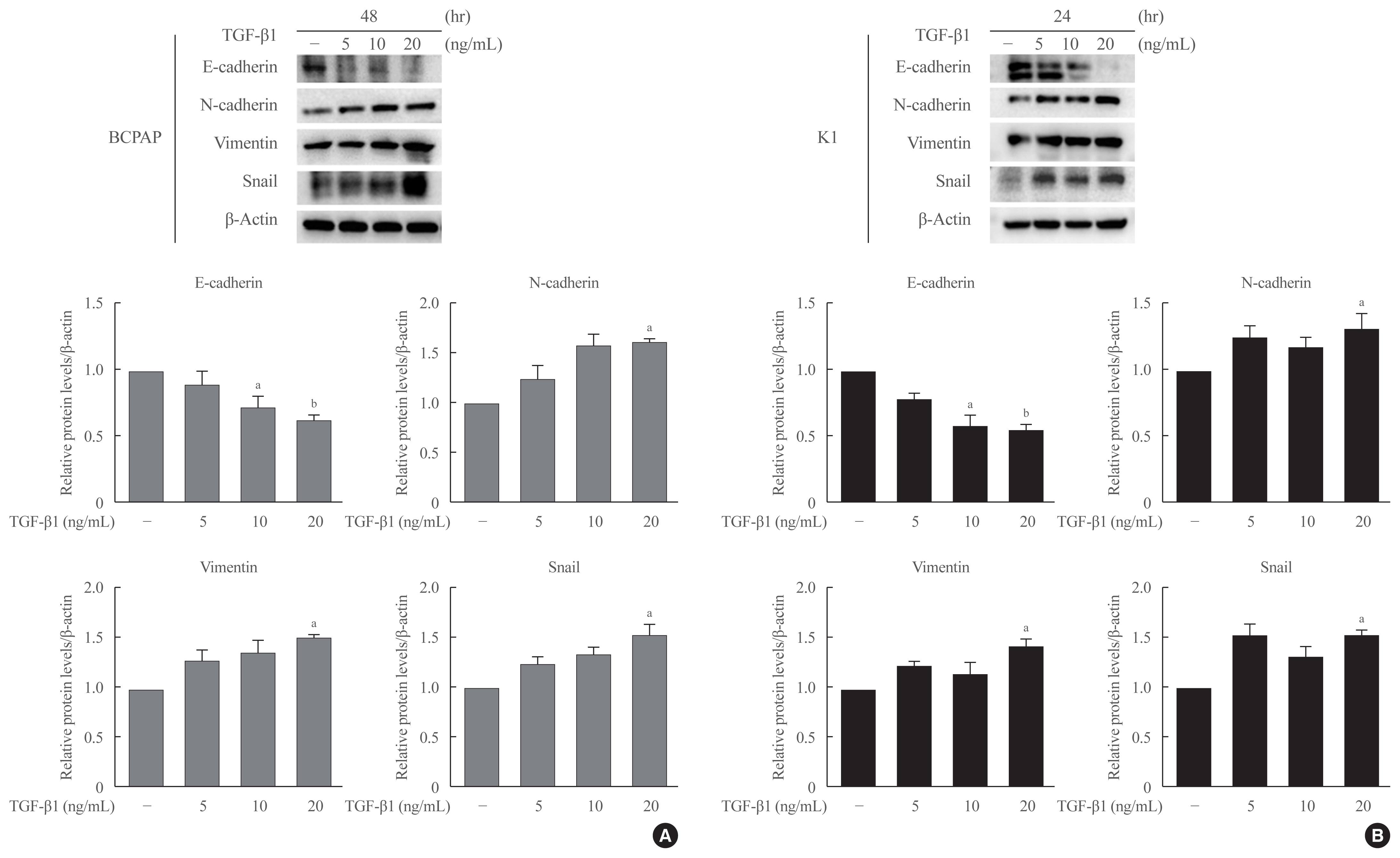
Half maximal inhibitory concentration (IC50) values of LGZ in BRAF-mutated PTC cell lines (BCPAP and K1) were determined using MTT assay. Rosiglitazone (RGZ), the PPAR-γ ligand was used as a positive control. The protein expression of PPAR-γ, cell-surface proteins (E-cadherin, N-cadherin), cytoskeletal protein (Vimentin), transcription factor (Snail), p38 mitogenactivated protein kinase (MAPK), extracellular signal-regulated kinase (ERK) 1/2 pathway, and matrix metalloproteinase (MMP)-2 expression were measured using Western blotting. Changes in E-cadherin expression were also determined using immunocytochemistry. Cell migration and invasion were analyzed using wound healing and Matrigel invasion assays.
Results
Treatment with LGZ or RGZ significantly inhibited transforming growth factor-beta1 (TGF-β1)-induced EMT-associated processes such as fibroblast-like morphological changes, EMT-related protein expression, and increased cell migration and invasion in BCPAP and K1 cells. LGZ restored TGF-β1-induced loss of E-cadherin, as observed using immunocytochemistry. Furthermore, LGZ and RGZ suppressed TGF-β1-induced MMP-2 expression and phosphorylation of p38 MAPK, but not ERK1/2. Although there was no change in PPAR-γ expression after treatment with LGZ or RGZ, the effect of downstream processes mediated by LGZ was hampered by GW9662, a PPAR-γ antagonist.
Conclusion
LGZ inhibits TGF-β1-induced EMT, migration, and invasion through the p38 MAPK signaling pathway in a PPAR-γ-dependent manner in PTC cells. -
Citations
Citations to this article as recorded by- Diabetes Mellitus and Thyroid Cancers: Risky Correlation, Underlying Mechanisms and Clinical Prevention
Rongqian Wu, Junping Zhang, Guilin Zou, Shanshan Li, Jinying Wang, Xiaoxinlei Li, Jixiong Xu
Diabetes, Metabolic Syndrome and Obesity.2024; Volume 17: 809. CrossRef - Clinicopathological Evaluation of Papillary Thyroid Microcarcinoma
Ando Takahito, Kimihito Fujii, Hirona Banno, Masayuki Saito, Yukie Ito, Mirai Ido, Manami Goto, Yukako Mouri, Junko Kousaka, Tsuneo Imai, Shogo Nakano
Cureus.2024;[Epub] CrossRef - Pioglitazone, a peroxisome proliferator‑activated receptor γ agonist, induces cell death and inhibits the proliferation of hypoxic HepG2 cells by promoting excessive production of reactive oxygen species
Guohao Huang, Mengfan Zhang, Manzhou Wang, Wenze Xu, Xuhua Duan, Xinwei Han, Jianzhuang Ren
Oncology Letters.2024;[Epub] CrossRef - The Activation of PPARγ by (2Z,4E,6E)-2-methoxyocta-2,4,6-trienoic Acid Counteracts the Epithelial–Mesenchymal Transition Process in Skin Carcinogenesis
Enrica Flori, Sarah Mosca, Giorgia Cardinali, Stefania Briganti, Monica Ottaviani, Daniela Kovacs, Isabella Manni, Mauro Truglio, Arianna Mastrofrancesco, Marco Zaccarini, Carlo Cota, Giulia Piaggio, Mauro Picardo
Cells.2023; 12(7): 1007. CrossRef - Cumulative exposure to metabolic syndrome increases thyroid cancer risk in young adults: a population-based cohort study
Jinyoung Kim, Kyungdo Han, Mee Kyoung Kim, Ki-Hyun Baek, Ki-Ho Song, Hyuk-Sang Kwon
The Korean Journal of Internal Medicine.2023; 38(4): 526. CrossRef - Drug repositioning in thyroid cancer treatment: the intriguing case of anti-diabetic drugs
Alessia Greco, Francesca Coperchini, Laura Croce, Flavia Magri, Marsida Teliti, Mario Rotondi
Frontiers in Pharmacology.2023;[Epub] CrossRef - Fish and the Thyroid: A Janus Bifrons Relationship Caused by Pollutants and the Omega-3 Polyunsaturated Fatty Acids
Salvatore Benvenga, Fausto Famà, Laura Giovanna Perdichizzi, Alessandro Antonelli, Gabriela Brenta, Francesco Vermiglio, Mariacarla Moleti
Frontiers in Endocrinology.2022;[Epub] CrossRef - Identifying and categorizing compounds that reduce corneal transforming growth factor beta induced protein levels: a scoping review
Gabriella Guo Sciriha, Janet Sultana, Joseph Borg
Expert Review of Clinical Pharmacology.2022; 15(12): 1423. CrossRef
- Diabetes Mellitus and Thyroid Cancers: Risky Correlation, Underlying Mechanisms and Clinical Prevention

- Hypothalamus and Pituitary Gland
- Heart Rate Variability in Postoperative Patients with Nonfunctioning Pituitary Adenoma
- Jeonghoon Ha, Hansang Baek, Chaiho Jeong, Minsoo Yeo, Seung-Hwan Lee, Jae Hyoung Cho, Ki-Hyun Baek, Moo Il Kang, Dong-Jun Lim
- Endocrinol Metab. 2021;36(3):678-687. Published online June 10, 2021
- DOI: https://doi.org/10.3803/EnM.2021.978
- 4,549 View
- 109 Download
- 3 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Decreased heart rate variability (HRV) has been reported to be associated with cardiac autonomic dysfunction. Hypopituitarism in nonfunctioning pituitary adenoma (NFPA) is often linked to increased cardiovascular mortality. We therefore hypothesized that postoperative NFPA patients with hormone deficiency have an elevated risk of HRV alterations indicating cardiac autonomic dysfunction.
Methods
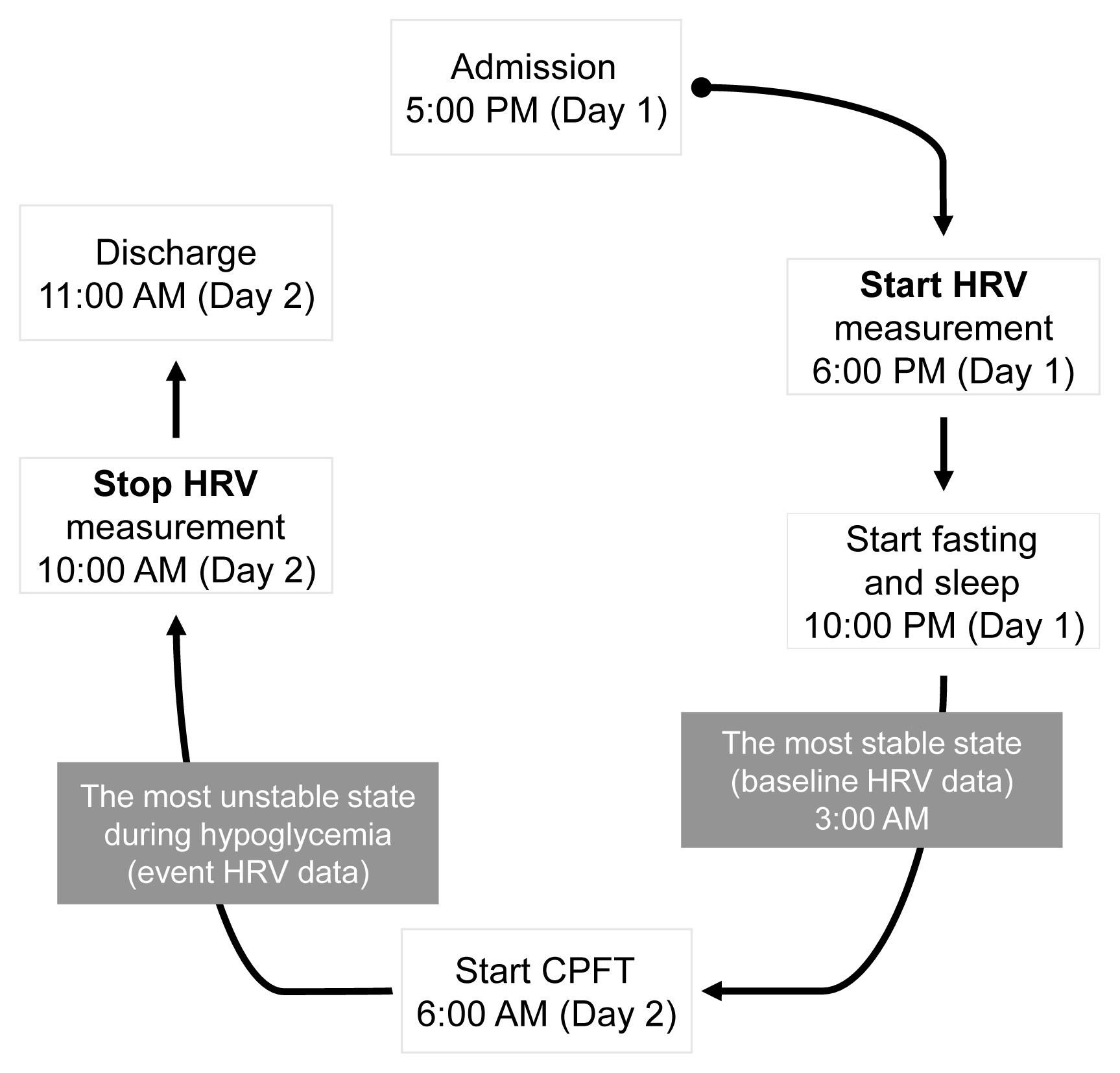
A total of 22 patients with NFPA were enrolled in the study. Between 3 and 6 months after surgery, a combined pituitary function test (CPFT) was performed, and HRV was measured. The period of sleep before the CPFT was deemed the most stable period, and the hypoglycemic period that occurred during the CPFT was defined as the most unstable period. Changes in HRV parameters in stable and unstable periods were observed and compared depending on the status of hormone deficiencies.
Results
In patients with adrenocorticotropic hormone (ACTH) deficiency with other pituitary hormone deficiencies, the low frequency to high frequency ratio, which represents overall autonomic function and is increased in the disease state, was higher (P=0.005). Additionally, the standard deviation of the normal-to-normal interval, which decreases in the autonomic dysfunction state, was lower (P=0.030) during the hypoglycemic period. In panhypopituitarism, the low frequency to high frequency ratio during the hypoglycemic period was increased (P=0.007).
Conclusion
HRV analysis during CPFT enables estimation of cardiac autonomic dysfunction in patients with NFPA who develop ACTH deficiency with other pituitary hormone deficiencies or panhypopituitarism after surgery. These patients may require a preemptive assessment of cardiovascular risk. -
Citations
Citations to this article as recorded by- Heart Rate Variability in Subjects with Severe Allergic Background Undergoing COVID-19 Vaccination
Maria Bernadette Cilona, Filippo D’Amico, Chiara Asperti, Giuseppe Alvise Ramirez, Stefano Turi, Giovanni Benanti, Shai Marc Bohane, Serena Nannipieri, Rosa Labanca, Matteo Gervasini, Federica Russetti, Naomi Viapiana, Martina Lezzi, Giovanni Landoni, Lor
Vaccines.2023; 11(3): 567. CrossRef - Pituitary Diseases and COVID-19 Outcomes in South Korea: A Nationwide Cohort Study
Jeonghoon Ha, Kyoung Min Kim, Dong-Jun Lim, Keeho Song, Gi Hyeon Seo
Journal of Clinical Medicine.2023; 12(14): 4799. CrossRef - Effect of a 16-Session Qigong Program in Non-Hodgkin Lymphoma Survivors: A Randomized Clinical Trial
Keyla Vargas-Román, Emilia I. De la Fuente-Solana, Jonathan Cortés-Martín, Juan Carlos Sánchez-García, Christian J. González-Vargas, Lourdes Díaz-Rodríguez
Journal of Clinical Medicine.2022; 11(12): 3421. CrossRef
- Heart Rate Variability in Subjects with Severe Allergic Background Undergoing COVID-19 Vaccination

- Clinical Study
- Association of Hyperparathyroidism and Papillary Thyroid Cancer: A Multicenter Retrospective Study
- Chaiho Jeong, Hye In Kwon, Hansang Baek, Hun-Sung Kim, Dong-Jun Lim, Ki-Hyun Baek, Jeonghoon Ha, Moo Il Kang
- Endocrinol Metab. 2020;35(4):925-932. Published online December 10, 2020
- DOI: https://doi.org/10.3803/EnM.2020.725
- 5,339 View
- 183 Download
- 9 Web of Science
- 8 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
Concomitant papillary thyroid cancer (PTC) and hyperparathyroidism (HPT) have been reported in several studies. Our study aimed to investigate the incidence of concomitant PTC in HPT patients upon preoperative diagnosis and present a clinical opinion on detecting thyroid malignancy in case of parathyroidectomy.
Methods
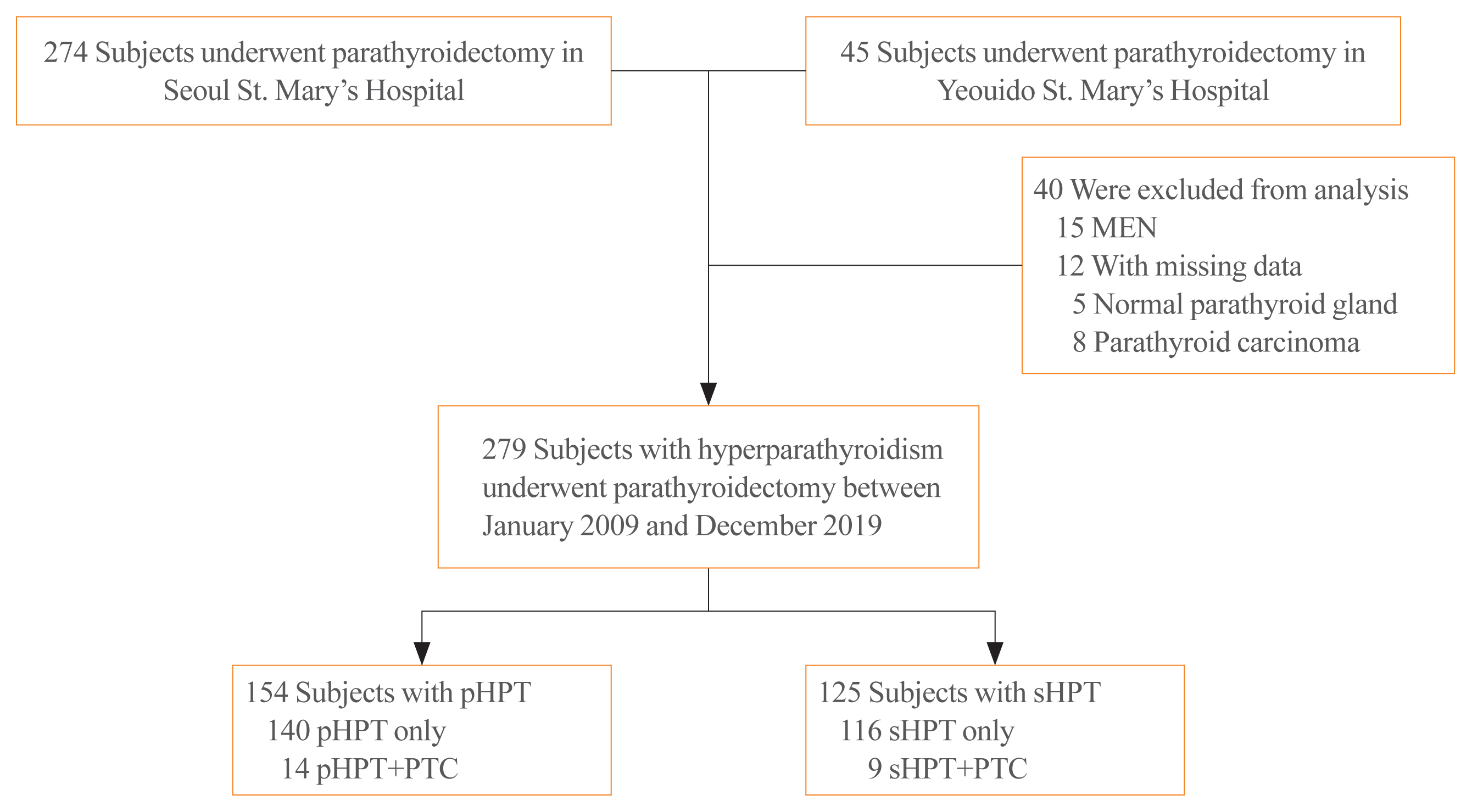
Patients who underwent parathyroidectomy between January 2009 and December 2019 in two medical centers were included. Of the 279 participants 154 were diagnosed as primary hyperparathyroidism (pHPT) and 125 as secondary hyperparathyroidism (sHPT). The incidence of concomitant PTC and its clinical characteristics were compared with 98 patients who underwent thyroidectomy and were diagnosed with classical PTC during the same period.
Results
Concurrent PTC was detected in 14 patients (9.1%) with pHPT and in nine patients (7.2%) with sHPT. Ten (71.4%) and seven (77.8%) PTCs were microcarcinomas in the pHPT and sHPT cases respectively. In the pHPT patients, vitamin D was lower in the pHPT+PTC group (13.0±3.7 ng/mL) than in the pHPT-only group (18.5±10.4 ng/mL; P=0.01). Vitamin D levels were also lower in the sHPT+PTC group (12.3±5.6 ng/mL) than in the sHPT-only group (18.0±10.2 ng/mL; P=0.12). In the concomitant PTC group, lymph node ratio was higher than in the classical PTC group (P=0.00).
Conclusion
A high prevalence of concomitant PTC was seen in patients with pHPT and sHPT. Those concomitant PTCs were mostly microcarcinomas and had more aggressive features, suggesting that efforts should be made to detect concomitant malignancies in the preoperative parathyroidectomy evaluation. -
Citations
Citations to this article as recorded by- The unexpected effect of parathyroid adenoma on inflammation
Ahmet Tarik Harmantepe, Belma Kocer, Zulfu Bayhan, Emre Gonullu, Ugur Can Dulger
Updates in Surgery.2024; 76(2): 589. CrossRef - Evaluation of Nodular Goiter and Papillary Thyroid Cancer Coincidence in Patients with Primary Hyperparathyroidism
Mustafa ÇALIŞKAN, Hasret CENGİZ, Taner DEMİRCİ
Düzce Tıp Fakültesi Dergisi.2023; 25(2): 200. CrossRef - Papillary thyroid carcinoma coexisting with benign thyroid and parathyroid pathology: clinical and pathomorphological features
A. Dinets, M. Gorobeiko, V. Hoperia, A. Lovin, S. Tarasenko
INTERNATIONAL JOURNAL OF ENDOCRINOLOGY (Ukraine).2023; 19(4): 274. CrossRef - The Nexus of Hyperparathyroidism and Thyroid Carcinoma: Insights into Pathogenesis and Diagnostic Challenges—A Narrative Review
Gregorio Scerrino, Nunzia Cinzia Paladino, Giuseppina Orlando, Giuseppe Salamone, Pierina Richiusa, Stefano Radellini, Giuseppina Melfa, Giuseppa Graceffa
Journal of Clinical Medicine.2023; 13(1): 147. CrossRef - Is preoperative parathyroid localization necessary for tertiary hyperparathyroidism?
Rongzhi Wang, Peter Abraham, Brenessa Lindeman, Herbert Chen, Jessica Fazendin
The American Journal of Surgery.2022; 224(3): 918. CrossRef - Papillary thyroid carcinoma prevalence and its predictors in patients with primary hyperparathyroidism
Elif Tutku DURMUŞ, Ayşegül ATMACA, Mehmet KEFELİ, Ramis ÇOLAK, Buğra DURMUŞ, Cafer POLAT
Journal of Health Sciences and Medicine.2022; 5(5): 1499. CrossRef - Association of Hyperparathyroidism and Papillary Thyroid Cancer: A Multicenter Retrospective Study (Endocrinol Metab 2020;35:925-32, Chaiho Jeong et al.)
Chaiho Jeong, Jeonghoon Ha, Moo Il Kang
Endocrinology and Metabolism.2021; 36(1): 205. CrossRef - Association of Hyperparathyroidism and Papillary Thyroid Cancer: A Multicenter Retrospective Study (Endocrinol Metab 2020;35:925-32, Chaiho Jeong et al.)
Burcu Candemir, Coşkun Meriç
Endocrinology and Metabolism.2021; 36(1): 203. CrossRef
- The unexpected effect of parathyroid adenoma on inflammation

- Thyroid
- Cholestyramine Use for Rapid Reversion to Euthyroid States in Patients with Thyrotoxicosis
- Jeonghoon Ha, Kwanhoon Jo, Borami Kang, Min-Hee Kim, Dong-Jun Lim
- Endocrinol Metab. 2016;31(3):476-479. Published online July 26, 2016
- DOI: https://doi.org/10.3803/EnM.2016.31.3.476
- 3,881 View
- 51 Download
- 6 Web of Science
- 7 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Cholestyramine (CS) is an ion exchange resin, which binds to iodothyronines and would lower serum thyroid hormone level. The use of CS added to conventional antithyroid drugs to control thyrotoxicosis has been applied since 1980's, and several studies indicate that using CS in combination with methimazole (MZ) produces a more rapid decline in serum thyroid hormones than with only MZ treatment. Our recent retrospective review of five patients taking high dose MZ and CS, compared to age-, gender-, initial free thyroxine (T4) level-, and MZ dose-matched 12 patients with MZ use only, showed more rapid decline of both free T4 and triiodothyronine levels without more adverse events. CS could be safely applicable short-term adjunctive therapy when first-line antithyroid medications are not enough to adequately control severe thyrotoxicosis or side effects of antithyroid drug would be of great concern.
-
Citations
Citations to this article as recorded by- Therapeutic plasma exchange for Graves’ disease in pregnancy
Matthew Lumchee, Mimi Yue, Josephine Laurie, Adam Morton
Obstetric Medicine.2023; 16(2): 126. CrossRef - Ventricular arrhythmias, antiarrhythmic therapy and thyroidal illness in advanced heart failure: a case report and review of the literature
Fatima Alsalama, Salma Alzaabi, Cynthia Salloum, Marilyne Abi Younes, Feras Bader, Hussam Ghalib, Bassam Atallah
Drugs & Therapy Perspectives.2023; 39(4): 147. CrossRef - Amiodarone Induced Thyrotoxicosis and Treatment Complications in a Man With Cyanotic Congenital Heart Disease: A Case Report
Marvin Wei Jie Chua, Shao Feng Mok
Frontiers in Cardiovascular Medicine.2020;[Epub] CrossRef - Propylthiouracil-induced agranulocytosis as a rare complication of antithyroid drugs in a patient with Graves’ disease
Patrícia Novais Rabelo, Paula Novais Rabelo, Allyne Fernanda de Paula, Samuel Amanso da Conceição, Daniela Pultrini Pereira de Oliveira Viggiano, Daniela Espíndola Antunes, Estela Muszkat Jatene, Sílvia Leda França Moura de Paula, Monike Lourenço Dias, Ma
Revista da Associação Médica Brasileira.2019; 65(6): 755. CrossRef - Notes on Trauma-Related Thyroid Storm in the Emergency Department
Adam Morton
The Journal of Emergency Medicine.2018; 54(2): e35. CrossRef - Risk of embryopathies with use of antithyroidal medications
Stine L. Andersen
Current Opinion in Endocrinology, Diabetes & Obesity.2017; 24(5): 364. CrossRef - Thiamazole
Reactions Weekly.2017; 1644(1): 291. CrossRef
- Therapeutic plasma exchange for Graves’ disease in pregnancy

- Thyroid
- Refractory Graves' Disease Successfully Cured by Adjunctive Cholestyramine and Subsequent Total Thyroidectomy
- Yeoree Yang, Seawon Hwang, Minji Kim, Yejee Lim, Min-Hee Kim, Sohee Lee, Dong-Jun Lim, Moo-Il Kang, Bong-Yun Cha
- Endocrinol Metab. 2015;30(4):620-625. Published online December 31, 2015
- DOI: https://doi.org/10.3803/EnM.2015.30.4.620
- 4,398 View
- 85 Download
- 15 Web of Science
- 13 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader The three major forms of treatment for Graves thyrotoxicosis are antithyroid drugs, radioactive iodine therapy and thyroidectomy. Surgery is the definitive treatment for Graves thyrotoxicosis that is generally recommended when other treatments have failed or are contraindicated. Generally, thyrotoxic patients should be euthyroid before surgery to minimize potential complications which usually requires preoperative management with thionamides or inorganic iodine. But several cases of refractory Graves' disease have shown resistance to conventional treatment. Here we report a 40-year-old female patient with Graves' disease who complained of thyrotoxic symptoms for 7 months. Her thyroid function test and thyroid autoantibody profiles were consistent with Graves' disease. One kind of thionamides and β-blocker were started to control her disease. However, she was resistant to nearly all conventional medical therapies, including β-blockers, inorganic iodine, and two thionamides. She experienced hepatotoxicity from the thionamides. What was worse is her past history of serious allergic reaction to corticosteroids, which are often used to help control symptoms. A 2-week regimen of high-dose cholestyramine improved her uncontrolled thyrotoxicosis and subsequent thyroidectomy was successfully performed. In conclusion, cholestyramine could be administered as an effective and safe adjunctive agent for preoperative preparation in patients with severe hyperthyroid Graves's disease that is resistant to conventional therapies.
-
Citations
Citations to this article as recorded by- Enhanced predictive validity of integrative models for refractory hyperthyroidism considering baseline and early therapy characteristics: a prospective cohort study
Xinpan Wang, Tiantian Li, Yue Li, Qiuyi Wang, Yun Cai, Zhixiao Wang, Yun Shi, Tao Yang, Xuqin Zheng
Journal of Translational Medicine.2024;[Epub] CrossRef - Non-thionamide antithyroid drug options in Graves’ hyperthyroidism
Aliya Ruslan, Onyebuchi E Okosieme
Expert Review of Endocrinology & Metabolism.2023; 18(1): 67. CrossRef - Gestione clinica dell’ipertiroidismo refrattario
Daniela Gallo, Federica Martina Bianchi, Francesca Manzella La Barbera, Ilaria Clementi, Adriana Lai, Eliana Piantanida, Maria Laura Tanda
L'Endocrinologo.2023; 24(2): 167. CrossRef - Carbimazole-Resistant Grave’s Thyrotoxicosis is a Diagnostic and Therapeutic Dilemma, Case Report with Literature Review
Fateen Ata, Adeel Ahmad Khan, Shuja Tahir, Zaina Al Amer
International Medical Case Reports Journal.2023; Volume 16: 783. CrossRef - Medical treatment of thyrotoxicosis
Lorenzo SCAPPATICCIO, Giuseppe BELLASTELLA, Maria I. MAIORINO, Luca GIOVANELLA, Katherine ESPOSITO
The Quarterly Journal of Nuclear Medicine and Molecular Imaging.2021;[Epub] CrossRef - THERAPEUTIC EFFECTS OF COMBINATION REGIMENS INCLUDING METHIMAZOLE ON GRAVES HYPERTHYROIDISM: A NETWORK META-ANALYSIS OF RANDOMIZED CONTROLLED TRIALS
Maorong Wang, Yerong Yu
Endocrine Practice.2020; 26(6): 675. CrossRef - Cholestyramine alters bile acid amounts and the expression of cholesterol‐related genes in rabbit intestinal and hepatic tissues
Dong Ni Qiu, Quan Shang, Da Yu Sun, Wei Qun Ding, Zhong Guang Luo, Jian Chen, Wei Ru Jiang, Jian Ping Huang, Xiao Yun Jiang
Journal of Digestive Diseases.2017; 18(2): 107. CrossRef - ENDOCRINOLOGY IN PREGNANCY: Pregnancy and the incidence, diagnosing and therapy of Graves’ disease
Peter Laurberg, Stine Linding Andersen
European Journal of Endocrinology.2016; 175(5): R219. CrossRef - 2016 American Thyroid Association Guidelines for Diagnosis and Management of Hyperthyroidism and Other Causes of Thyrotoxicosis
Douglas S. Ross, Henry B. Burch, David S. Cooper, M. Carol Greenlee, Peter Laurberg, Ana Luiza Maia, Scott A. Rivkees, Mary Samuels, Julie Ann Sosa, Marius N. Stan, Martin A. Walter
Thyroid.2016; 26(10): 1343. CrossRef - Cholestyramine Use for Rapid Reversion to Euthyroid States in Patients with Thyrotoxicosis
Jeonghoon Ha, Kwanhoon Jo, Borami Kang, Min-Hee Kim, Dong-Jun Lim
Endocrinology and Metabolism.2016; 31(3): 476. CrossRef - The role of bile acids in metabolic regulation
Libor Vítek, Martin Haluzík
Journal of Endocrinology.2016; 228(3): R85. CrossRef - Recent Advances in Autoimmune Thyroid Diseases
Won Sang Yoo, Hyun Kyung Chung
Endocrinology and Metabolism.2016; 31(3): 379. CrossRef - A Case of Methimazole-Resistant Severe Graves' Disease: Dramatic Response to Cholestyramine
Seung Byung Chae, Eun Sook Kim, Yun Im Lee, Bo Ram Min
International Journal of Thyroidology.2016; 9(2): 190. CrossRef
- Enhanced predictive validity of integrative models for refractory hyperthyroidism considering baseline and early therapy characteristics: a prospective cohort study

- Thyroid
- Accelerated Disease Progression after Discontinuation of Sorafenib in a Patient with Metastatic Papillary Thyroid Cancer
- Kyung-Jin Yun, Woohyeon Kim, Eun Hee Kim, Min-Hee Kim, Dong-Jun Lim, Moo-Il Kang, Bong-Yun Cha
- Endocrinol Metab. 2014;29(3):388-393. Published online September 25, 2014
- DOI: https://doi.org/10.3803/EnM.2014.29.3.388
- 3,551 View
- 30 Download
- 23 Web of Science
- 22 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Distant metastases from papillary thyroid carcinoma (PTC) are rare and are associated with a poor prognosis. Here, we describe a patient with metastatic PTC who was treated with a tyrosine kinase inhibitor (TKI, sorafenib) for several months that was acutely exacerbated by discontinuation. A 43-year-old male was diagnosed with PTC in February 2004 and underwent total thyroidectomy followed by two courses of high-dose radioactive iodine (RAI) therapy. Despite two additional courses of high-dose RAI therapy, lung and muscle metastases were developed. Treatment with sorafenib was begun in September 2010. After 11 months treatment of sorafenib, newly developed metastatic lesions were found in mediastinal lymph nodes, liver, and bones. Considered as treatment failure, the administration of sorafenib was discontinued. Two weeks after sorafenib treatment was stopped, the disease progressed abruptly and caused death of the patient by respiratory failure. In our patient, PTC progressed rapidly after the cessation of sorafenib treatment. Patients with several other types of cancer have also experienced such rapid disease progression, termed "flare-ups." Physicians should be aware that flare-ups may occur in advanced PTC patients following the cessation of TKI therapy.
-
Citations
Citations to this article as recorded by- Lenvatinib: an investigational agent for the treatment of differentiated thyroid cancer
Silvia Martina Ferrari, Giusy Elia, Francesca Ragusa, Sabrina Rosaria Paparo, Valeria Mazzi, Mario Miccoli, Maria Rosaria Galdiero, Gilda Varricchi, Rudy Foddis, Giovanni Guglielmi, Claudio Spinelli, Concettina La Motta, Salvatore Benvenga, Alessandro Ant
Expert Opinion on Investigational Drugs.2021; 30(9): 913. CrossRef - Low Dose of Lenvatinib Treatment for Patients of Radioiodine-Refractory Differentiated Thyroid Carcinoma – A Real-World Experience
He-Jiun Jiang, Yen-Hsiang Chang, Yen-Hao Chen, Che-Wei Wu, Pei-Wen Wang, Pi-Jung Hsiao
Cancer Management and Research.2021; Volume 13: 7139. CrossRef - Rapid disease progression after discontinuation of lenvatinib in thyroid cancer
Haruhiko Yamazaki, Kiminori Sugino, Kenichi Matsuzu, Chie Masaki, Junko Akaishi, Kiyomi Hames, Chisato Tomoda, Akifumi Suzuki, Takashi Uruno, Keiko Ohkuwa, Wataru Kitagawa, Mitsuji Nagahama, Munetaka Masuda, Koichi Ito
Medicine.2020; 99(11): e19408. CrossRef - Lenvatinib for thyroid cancer treatment: discovery, pre-clinical development and clinical application
Rosa Maria Paragliola, Andrea Corsello, Valeria Del Gatto, Giampaolo Papi, Alfredo Pontecorvi, Salvatore Maria Corsello
Expert Opinion on Drug Discovery.2020; 15(1): 11. CrossRef - Efficacy and Limitations of Lenvatinib Therapy for Radioiodine-Refractory Differentiated Thyroid Cancer: Real-World Experiences
Chie Masaki, Kiminori Sugino, Naoko Saito, Junko Akaishi, Kiyomi Y. Hames, Chisato Tomoda, Akifumi Suzuki, Kenichi Matsuzu, Takashi Uruno, Keiko Ohkuwa, Wataru Kitagawa, Mitsuji Nagahama, Koichi Ito
Thyroid.2020; 30(2): 214. CrossRef - Papillary thyroid carcinoma with hyperthyroidism and multiple metastases
Li-li Zhang, Bin Liu, Fang-fang Sun, Hong-yu Li, Shuang Li, Li-rong Zhao
Medicine.2020; 99(30): e21346. CrossRef - Missing Skeletal Muscle Metastases of Papillary Thyroid Carcinoma
Leszek Herbowski
Diagnostics.2020; 10(7): 457. CrossRef - Reply to “Missing Skeletal Muscle Metastases of Papillary Thyroid Carcinoma”
Liviu Hitu, Calin Cainap, Dragos Apostu, Katalin Gabora, Eduard-Alexandru Bonci, Marius Badan, Alexandru Mester, Andra Piciu
Diagnostics.2020; 10(7): 458. CrossRef - Hif-1α Inhibitors Could Successfully Inhibit the Progression of Differentiated Thyroid Cancer in Vitro
Min-Hee Kim, Tae Hyeong Lee, Jin Soo Lee, Dong-Jun Lim, Peter Chang-Whan Lee
Pharmaceuticals.2020; 13(9): 208. CrossRef - Extended Real-World Observation of Patients Treated with Sorafenib for Radioactive Iodine-Refractory Differentiated Thyroid Carcinoma and Impact of Lenvatinib Salvage Treatment: A Korean Multicenter Study
Hye-Seon Oh, Dong Yeob Shin, Mijin Kim, So Young Park, Tae Hyuk Kim, Bo Hyun Kim, Eui Young Kim, Won Bae Kim, Jae Hoon Chung, Young Kee Shong, Dong Jun Lim, Won Gu Kim
Thyroid.2019; 29(12): 1804. CrossRef - Rapid pleural effusion after discontinuation of lenvatinib in a patient with pleural metastasis from thyroid cancer
Taisuke Uchida, Hideki Yamaguchi, Kazuhiro Nagamine, Tadato Yonekawa, Eriko Nakamura, Nobuhiro Shibata, Fumiaki Kawano, Yujiro Asada, Masamitsu Nakazato
Endocrinology, Diabetes & Metabolism Case Reports.2019;[Epub] CrossRef - Thyroid Disorders in the Elderly
Kevin Higgins
Clinics in Geriatric Medicine.2018; 34(2): 259. CrossRef - Treatment of refractory thyroid cancer
Amandine Berdelou, Livia Lamartina, Michele Klain, Sophie Leboulleux, Martin Schlumberger, _ _
Endocrine-Related Cancer.2018; 25(4): R209. CrossRef - Clinical guidance for radioiodine refractory differentiated thyroid cancer
Matti L. Gild, Duncan J. Topliss, Diana Learoyd, Francis Parnis, Jeanne Tie, Brett Hughes, John P. Walsh, Donald S.A. McLeod, Roderick J. Clifton‐Bligh, Bruce G. Robinson
Clinical Endocrinology.2018; 88(4): 529. CrossRef - Case for Stopping Targeted Therapy When Lung Cancer Progresses on Treatment in Hospice-Eligible Patients
Thomas J. Smith, Nasser Hanna, David Johnson, Sherman Baker, William A. Biermann, Julie Brahmer, Peter M. Ellis, Giuseppe Giaccone, Paul J. Hesketh, Ishmael Jaiyesimi, Natasha B. Leighl, Gregory J. Riely, Joan H. Schiller, Bryan J. Schneider, Joan Tashbar
Journal of Oncology Practice.2017; 13(12): 780. CrossRef - Intermittent Dosing of Dabrafenib and Trametinib in Metastatic BRAFV600E Mutated Papillary Thyroid Cancer: Two Case Reports
Paul S. White, Anita Pudusseri, Stephanie L. Lee, Omar Eton
Thyroid.2017; 27(9): 1201. CrossRef - Aggressive differentiated thyroid cancer with multiple metastases and NRAS and TERT promoter mutations: A case report
Fabiana Pani, Elisabetta Macerola, Fulvio Basolo, Francesco Boi, Mario Scartozzi, Stefano Mariotti
Oncology Letters.2017; 14(2): 2186. CrossRef - Tumors Sharply Increased after Ceasing Pazopanib Therapy for a Patient with Advanced Uterine Leiomyosarcoma: Experience of Tumor Flare
Terumi Tanigawa, Shintaro Morisaki, Hisanobu Fukuda, Shuichiro Yoshimura, Hisayoshi Nakajima, Kohei Kotera
Case Reports in Obstetrics and Gynecology.2017; 2017: 1. CrossRef - Initial Size of Metastatic Lesions Is Best Prognostic Factor in Patients with Metastatic Differentiated Thyroid Carcinoma Confined to the Lung
Mijin Kim, Won Gu Kim, Suyeon Park, Hyemi Kwon, Min Ji Jeon, Jong Jin Lee, Jin-Sook Ryu, Tae Yong Kim, Young Kee Shong, Won Bae Kim
Thyroid.2017; 27(1): 49. CrossRef - Articles in 'Endocrinology and Metabolism' in 2014
Won-Young Lee
Endocrinology and Metabolism.2015; 30(1): 47. CrossRef - Pharmacodynamic study of axitinib in patients with advanced malignancies assessed with 18F-3′deoxy-3′fluoro-l-thymidine positron emission tomography/computed tomography
Justine Yang Bruce, Peter Colin Scully, Lakeesha L. Carmichael, Jens C. Eickhoff, Scott B. Perlman, Jill Marie Kolesar, Jennifer L. Heideman, Robert Jeraj, Glenn Liu
Cancer Chemotherapy and Pharmacology.2015; 76(1): 187. CrossRef - Optimal Differentiated Thyroid Cancer Management in the Elderly
Donald S. A. McLeod, Kelly Carruthers, Dev A. S. Kevat
Drugs & Aging.2015; 32(4): 283. CrossRef
- Lenvatinib: an investigational agent for the treatment of differentiated thyroid cancer


 KES
KES

 First
First Prev
Prev



